Measles Resurgence 2026: Your Essential Health Action Plan Amidst Rising Cases
 Protecting communities against the global measles resurgence requires collective action and informed health strategies.This image is a visual representation and it is not intended to provide medical advice or endorse specific products or services. Consult with a qualified healthcare professional for personalized health information and recommendations.
Protecting communities against the global measles resurgence requires collective action and informed health strategies.This image is a visual representation and it is not intended to provide medical advice or endorse specific products or services. Consult with a qualified healthcare professional for personalized health information and recommendations.The Shadow of Resurgence: Understanding the 2025-2026 Measles Crisis
The year 2026 presents a stark irony in global health. As we celebrate breakthroughs in genomic sequencing and automated diagnostics, a foundational pillar of pediatric well-being—routine immunization—is experiencing its most significant regression in half a century. The measles (rubeola) surge of 2025 and 2026 is more than a localized spike; it's a systemic failure of health security, breaching the borders of nearly 100 countries and revoking the hard-won elimination status of nations once thought immune. This isn't a phenomenon that occurred in a vacuum; it's the culmination of a "perfect storm" fueled by declining vaccination rates, record-high non-medical exemptions, and a strategic withdrawal from global health partnerships [3].
While the World Health Organization (WHO) and UNICEF reported a 75% decline in European and Central Asian cases in 2025 compared to the record-breaking 127,412 cases in 2024, they simultaneously warned that this progress remains "fragile" [5]. The reduction was largely due to aggressive, resource-intensive outbreak response measures rather than a stabilization of routine coverage, which stubbornly remains below the critical 95% threshold required for herd immunity [5]. This delicate balance means that even minor shifts can lead to widespread outbreaks, making vigilance absolutely crucial.
"While measles cases dropped in Europe and Central Asia in 2025 compared to the previous year, the risk of outbreaks remains 'fragile' due to coverage below the 95% herd immunity threshold."
Insight You Can Use:
Recognize that even reported declines in measles cases might not reflect a stable improvement in population immunity. Always verify vaccination rates and local public health advisories, especially if traveling to or from regions with historical outbreaks, as a seemingly contained situation can quickly become precarious.
The Global Epidemiological Landscape: A Comparative Analysis
From 2024 to early 2026, the epicenter of measles transmission has dramatically shifted. In 2024, the European Region bore a significant portion of the global burden, accounting for one-third of all cases [8]. However, by 2025, the crisis had intensified across the Americas and specific hotspots in the African and Eastern Mediterranean regions. The Pan American Health Organization (PAHO) recorded a staggering 34-fold increase in measles cases in the Americas during the first eight months of 2025 compared to the same period in 2024 [9]. This surge underlines the highly contagious nature of the virus and its ability to exploit immunity gaps.
The American continent's experience in 2025 serves as a cautionary tale. After being declared free of endemic measles in 2016—a milestone unique among WHO regions—the Americas have witnessed a catastrophic reversal [9]. Canada's loss of elimination status, for instance, was driven by a sustained outbreak among undervaccinated communities, particularly the Mennonite populations, which then fueled clusters across several neighboring countries. This cross-border transmission highlights the biological reality: measles is one of the most contagious airborne pathogens, with a secondary attack rate of 90% among susceptible close contacts [1].
In the United States, the surge has been equally alarming. By the end of May 2025, the country had already exceeded 1,000 cases, predominantly in undervaccinated clusters in Texas, New Mexico, and Oklahoma [14]. This momentum continued into 2026, with nearly 1,000 cases reported in just the first two months, centered in states like South Carolina, Utah, Arizona, and Florida [11]. The demographic breakdown of these cases is telling: 93% to 94% of infected individuals were unvaccinated or had unknown vaccination status, unequivocally emphasizing that the surge is primarily a crisis of non-immunization [10].
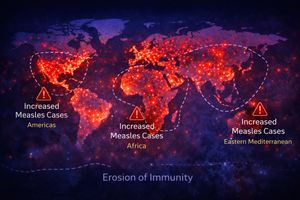 The global measles landscape in 2025-2026 reflects a concerning shift in transmission epicenters.This image is a visual representation and it is not intended to provide medical advice or endorse specific products or services. Consult with a qualified healthcare professional for personalized health information and recommendations.
The global measles landscape in 2025-2026 reflects a concerning shift in transmission epicenters.This image is a visual representation and it is not intended to provide medical advice or endorse specific products or services. Consult with a qualified healthcare professional for personalized health information and recommendations."Ten countries in the Americas reported measles outbreaks in 2025, with a 34-fold increase compared to the same period in 2024."
Next Move to Consider:
If you reside in or plan to travel to regions experiencing measles outbreaks, check your vaccination records immediately. Ensure all family members, especially children and those born after 1957, have received two doses of the MMR vaccine. For infants aged 6-12 months traveling internationally, consult a pediatrician about an early MMR dose.
Pathophysiology and the Clinical Impact of Immune Amnesia
The 2025-2026 measles surge has provided a grim opportunity for researchers to delve deeper into the long-term clinical sequelae of rubeola, extending beyond the acute phase. While the public often perceives measles as a relatively benign childhood illness characterized by a transient rash and fever, clinicians are increasingly focused on the "shadow of mortality" cast by the virus through a phenomenon known as immune amnesia [6].
The Mechanism of Immunological Erosion
Measles is caused by a single-stranded RNA paramyxovirus that specifically targets the CD150 (SLAM) receptor found on the surface of lymphoid and myeloid cells [16]. Upon infection, the virus infiltrates memory T cells and follicular B cells—the "special forces" of the immune system that store information on how to fight previously encountered pathogens [17]. Research conducted during the 2025 Texas outbreak and published in early 2026 identifies a three-step process for this immunological destruction:
- Viremic Infiltration: The virus enters the bone marrow and infects long-lived plasma B cells, which are non-dividing "factories" producing antibodies against diseases like influenza, RSV, and chickenpox [16].
- Cellular Clearance: The host's own immune system then identifies and destroys these infected memory cells to clear the measles virus, effectively purging the body's immunological library [17].
- The Naive Repopulation: As the body recovers, it produces new immune cells, but these are primarily "naive" (having no experience with other germs) or exclusively specific to the measles virus. The individual must essentially "start over" and retrain their immune system through new exposures or re-vaccination [16].
Quantitative analysis using specialized antibody detection in blood samples has shown that even mild cases of measles result in the loss of 33% of the preexisting antibody repertoire [16]. Severe cases can lead to a 40% loss [16]. This loss is stable and does not recover on its own, leaving the survivor vulnerable to secondary infections for up to three years [16]. This "immune amnesia" is a critical, often overlooked consequence of measles infection.
Clinical Precaution:
Understand that surviving measles doesn't mean you're in the clear; your immune system may be compromised for years. If you've had measles, be extra vigilant about other infections and discuss with your healthcare provider whether any booster vaccinations for other diseases are advisable, as your previous immunity may have been "erased."
Diagnostic Evolution: PCR vs. Serology in High Vaccination Settings
As the 2025-2026 surge progressed, the limitations of traditional diagnostic methods became a significant barrier to effective outbreak control. The presence of partially vaccinated individuals and the emergence of "modified measles" presentations (milder symptoms due to partial immunity) have necessitated a transition toward more sensitive molecular techniques [24].
The Failure of Traditional Serology
Historically, the detection of measles-specific IgM antibodies was the gold standard for diagnosis. However, in 2026, relying solely on IgM is considered problematic for several reasons:
- Vaccinated Breakthroughs: In individuals who have received one or two doses of the MMR vaccine but still contract the virus (modified measles), the IgM response is often transient, delayed, or entirely absent [24].
- Low Predictive Value: In regions where measles is rare, the positive predictive value of an IgM test is exceedingly low, as many other viruses can cause false-positive results [24].
- Timing Sensitivity: IgM may not be detectable until at least 72 hours after the rash onset, creating a window where an infected person may test negative while actively spreading the virus [20].
The Shift to Real-Time RT-PCR (rRT-PCR)
The 2026 guidelines from the CDC and the Oregon State Public Health Laboratory (OSPHL) now emphasize rRT-PCR as the preferred confirmatory testing method [19]. PCR remains highly sensitive even in breakthrough cases where viral loads may be lower and clear more rapidly than in primary infections [24].
Furthermore, the recent analytical validation of dual-target RT-PCR (dt-MeV) assays on automated systems like the Hologic Panther Fusion represents a major breakthrough [25]. These assays allow for the simultaneous detection of the virus and the differentiation between wild-type and vaccine strains. The ability to distinguish between vaccine-derived strains (genotype A) and wild-type virus is critical for public health resource management. Individuals presenting with a rash shortly after receiving the MMR vaccine do not require airborne isolation or intensive contact tracing, as the vaccine strain is not considered contagious [25]. Without such differentiation, health departments often find themselves "over-responding" to vaccine-induced side effects, diverting critical staff from actual wild-type outbreaks.
Practical Steps You Can Apply:
If you suspect measles, especially after recent travel or exposure, advocate for PCR testing over traditional antibody tests. Inform your healthcare provider about your vaccination history and any recent MMR shots, as this context is crucial for accurate diagnosis and preventing unnecessary isolation measures.
The Perfect Storm: Leadership, Funding, and Public Health Infrastructure
The 2025-2026 surge is not merely a biological phenomenon; it is a manifestation of the "dismantling of public health" [3]. This period has seen a dramatic shift in federal and international health policy that has weakened the global immune system.
The Impact of Infrastructure Dismantling
In March 2025, the U.S. federal government terminated $11.4 billion in grants intended for state and local health departments [3]. This withdrawal crippled the ability of local jurisdictions to conduct the labor-intensive work of measles control. In Dallas, for instance, budget cuts led to the cancellation of 50 mobile vaccination clinics and the loss of 21 epidemiology staff members precisely when cases were surging in neighboring counties [3].
The consequences of this withdrawal extended globally. Decisions to terminate funding for the WHO Global Measles and Rubella Laboratory Network (which includes over 700 laboratories in 150 countries) and the end of U.S. financial support for Gavi, the Vaccine Alliance, have created an environment where the "virus never rests" while its primary adversaries are being defunded [3]. This erosion of infrastructure makes rapid response and surveillance significantly more challenging.
The Changing Political Climate and Vaccine Hesitancy
The political landscape in 2025-2026 has increasingly prioritized individual liberty and skepticism of scientific institutions over collective health security. Leaders at the highest levels of the Health and Human Services (HHS) department have promoted narratives that frame childhood vaccination as a "personal choice" while downplaying the risk of transmission to the vulnerable [3].
This shift has had a measurable impact on public behavior:
- Declining Coverage: National 2-dose MMR coverage in the U.S. fell from 95.2% in 2019-20 to 92.7% in 2023-24 [3].
- Record-High Exemptions: Non-medical exemptions for kindergarteners reached a record high of 3.3% in 2025, with 14 states reporting exemption rates exceeding 5%—the threshold that makes herd immunity mathematically impossible [3].
- Erosion of Trust: Polls in 2025 showed that 25% of parents now believe the risks of childhood vaccines outweigh their benefits, while trust in state and local health officials has fallen to 46% among some demographics [3].
The "Perfect Storm" is thus defined by the convergence of biological high-infectivity, declining population immunity, and a paralyzed public health apparatus. In Gaines County, Texas, where MMR coverage among kindergarteners fell to 82%, the measles virus found an ideal environment to establish a foothold and spread across state lines into New Mexico and Oklahoma [3].
Key Lesson for Your Workflow:
Be aware that reduced public health funding and declining vaccination rates create local immunity gaps. If you're a healthcare provider, redouble efforts to educate parents on vaccine safety and efficacy, and advocate for restoring public health funding. If you're a parent, critically evaluate information and prioritize official health recommendations.
The Digital Contagion: Debunking Platform-Specific Misinformation
Parallel to the physical spread of the virus is the digital spread of misinformation. The 2025-2026 surge has been fueled by sophisticated narratives on platforms like TikTok and WhatsApp, which often outperform verified health information in engagement metrics.
TikTok and the "Eco-Influencer" Movement
Research presented at the American Academy of Pediatrics 2025 National Conference highlighted the rise of "eco-influencers" who promote "natural living" and alternative medical parenting [26]. A study of 120 high-engagement TikTok videos using hashtags like #naturalparenting and #alternativehealing found that 61% contained information that directly contradicted pediatric guidelines [26]. The "whack-a-mole" metaphor used by public health experts to describe online misinformation remains accurate in 2026; 80% of misinformation content created by self-identified parents and influencers carries more weight with some audiences than content from healthcare professionals [15].
Debunking the Vitamin A Narrative
A particularly dangerous trend in 2025-2026 is the promotion of Vitamin A as a preventative alternative to the MMR vaccine. This narrative gained prominence when HHS leadership emphasized "good nutrition" alone as adequate protection [3]. While Vitamin A is a recommended supportive treatment for children already diagnosed with severe measles—as it can reduce the severity of complications and risk of blindness—it is not a substitute for vaccination [15]. The overuse of Vitamin A in healthy children has led to reports of toxicity in Texas, causing damage to the liver, bones, and central nervous system [3]. Public health agencies in 2026 are forced to clarify that two doses of the MMR vaccine provide 97% lifelong protection, a level of security that nutrition alone cannot provide [7].
Social Strategy:
Be a critical consumer of online health information. Always cross-reference claims, especially those promoting alternative treatments, with reputable sources like the CDC or WHO. If you see misinformation, report it and share accurate information from verified health organizations to help counter the digital contagion.
Global Health Security and 2026 Travel/Isolation Policies
The ease of international travel remains the primary mechanism for the "importation" of measles into eliminated zones. In 2025 and 2026, travel-associated cases have been the catalyst for nearly all major outbreaks in the United States and Canada [1].
Updated 2026 Travel Advisories
The 2026 edition of the CDC Yellow Book and IATA medical manuals have updated their requirements to reflect the increased global risk. Healthcare professionals are now advised to consider measles in any patient presenting with fever and rash, particularly if they have traveled domestically or internationally to an outbreak area within the last 21 days [13].
For international travelers, the 2026 recommendations are specific:
- Infants (6–12 months): Should receive one dose of the MMR vaccine before travel. This dose is considered "pre-routine" and must be followed by the standard two-dose series after their first birthday [29].
- Children and Adults: Must have written documentation of two doses of the MMR vaccine separated by at least 28 days [21].
- Timing: Vaccination should be completed at least two weeks before travel to ensure maximum antibody production [29].
 Updated travel advisories in 2026 underscore the critical need for pre-travel MMR vaccination for all ages.This image is a visual representation and it is not intended to provide medical advice or endorse specific products or services. Consult with a qualified healthcare professional for personalized health information and recommendations.
Updated travel advisories in 2026 underscore the critical need for pre-travel MMR vaccination for all ages.This image is a visual representation and it is not intended to provide medical advice or endorse specific products or services. Consult with a qualified healthcare professional for personalized health information and recommendations.Isolation and Biosecurity Protocols
In 2026, isolation protocols for suspected cases have become more stringent to prevent transmission in healthcare settings. If a patient presents with symptoms, they are not to be kept in common waiting rooms. Instead, they must be moved immediately to a single-patient airborne infection isolation room (AIIR) [21].
Healthcare workers without proof of immunity who are exposed to the virus are now excluded from the workplace starting from Day 5 after their first exposure until Day 21 after their last exposure [28]. This "5-to-21" rule is critical because a person is contagious for four days before the rash appears, making asymptomatic transmission a primary driver of the current surge [1]. For air travel, the IATA 2026 guidelines recommend that cabin crew isolate symptomatic passengers as far as possible from others and treat all respiratory secretions as potentially infectious. The use of the Passenger Locator Form (PLF) is now a standard requirement for any flight where a suspected case is identified, allowing local health departments to conduct rapid contact tracing for passengers seated in the immediate vicinity [33].
Next Move to Consider:
Before any international or domestic travel, especially during an outbreak, confirm your and your family's MMR vaccination status. Be prepared for enhanced screening and isolation protocols if you develop symptoms, and always declare recent travel history to healthcare providers immediately.
Forecasting and Scenario-Based Modeling for 2026-2027
Mathematical modeling conducted by researchers at Imperial College London and the London School of Hygiene and Tropical Medicine (LSHTM) provides a sobering vision of the potential future of the measles resurgence [35].
The Shift Toward Adult Susceptibility
A key finding of 2026 modeling is that measles is no longer strictly a "childhood disease." In Europe and the Americas, between 25% and 50% of cases observed since 2015 have occurred in older teenagers and adults [35]. This shift is attributed to "pockets of susceptibility" in cohorts born in the late 1990s and early 2000s, who may have missed vaccination due to the historical surge in misinformation during that era [35]. Recent adjustments to these models emphasize that the threshold for herd immunity may actually be higher than 95% in settings with high migration and dense adult contact networks [4].
Long-Term Economic and Mortality Scenarios
Scenario analysis for the next two decades suggests that if vaccination coverage does not rebound to pre-pandemic levels, the United Kingdom could experience nearly 400,000 additional cases and 480 deaths, with economic losses exceeding £290 million [37]. In the United States, current models suggest that the loss of elimination status in 2026 is a "high-probability" event if the current pace of outbreaks in the Americas continues [1]. These models demonstrate that measles transmission is not a static threat; the virus is adept at finding "unprotected bridges" between undervaccinated communities. As social interaction patterns normalized in 2024-2025, the largest number of outbreaks since 2003 was recorded, indicating that the window for re-establishing control is rapidly closing [4].
"If vaccination coverage does not rebound, the UK could experience nearly 400,000 additional cases and 480 deaths over the next two decades."
Fiscal Move to Make:
Support public health initiatives and vaccination campaigns, not just for children but also for at-risk adults. The long-term economic and human costs of unchecked measles outbreaks far outweigh the investment in robust vaccination programs and public health infrastructure.
Investigative Conclusion: The Imperative for Integrated Action
The 2025-2026 measles surge is a multi-dimensional crisis that defies simple solutions. The biological high-infectivity of the virus, with an R0 of up to 18, means that even a minor slippage in public health vigilance translates into a catastrophic loss of control [7]. Our investigation into this resurgence reveals a fundamental truth: public health victories are never permanent [14].
The clinical reality of immune amnesia provides the most compelling argument for a renewed focus on vaccination. By preventing measles, the medical community is not just stopping a single virus; it is preserving the immunological memory of the entire human species. The "shadow of mortality" that follows an outbreak can only be dispelled through the restoration of herd immunity and the stabilization of the health systems that support it.
To reverse the regression seen in 2025-2026, the following imperatives are clear:
- Diagnostic Modernization: Wide-scale deployment of dual-target PCR assays to accurately classify cases and manage resources [25].
- Infrastructure Reinforcement: Restoration of funding for surveillance and the global laboratory network to ensure that "the virus never rests" alone [3].
- Communication Innovation: Moving beyond "whack-a-mole" misinformation response toward a proactive engagement with the communities most affected by vaccine hesitancy [15].
- Policy Realism: Recognizing that elimination is an epidemiological victory that can only last as long as the 95% coverage threshold is maintained [1].
The current surge is a "wake-up call" for global health security [8]. As the world moves deeper into 2026, the cost of inaction is measured not just in measles cases, but in the erosion of the collective protection that has saved millions of lives over the past century. The path forward requires a return to the evidence-based strategies that once made measles elimination a reality, combined with a modern understanding of the digital and biological complexities of the 21st century.
Next Steps You Can Take:
Act now by ensuring your family's vaccination records are up-to-date, engaging respectfully in vaccine discussions, and supporting policies that strengthen public health infrastructure. Your proactive choices contribute to community-wide protection against this highly contagious and debilitating disease.
Frequently Asked Questions About the 2026 Measles Outbreak and Your Health
What is immune amnesia and how does measles cause it?
Why is RT-PCR preferred over traditional serology for measles diagnosis now?
Can adults get measles, and what are their specific risks in the current resurgence?
Is Vitamin A a suitable alternative to the MMR vaccine for measles prevention?
What is the "5-to-21" rule for healthcare workers exposed to measles, and why is it important?
Disclaimer: This article addresses health-related topics for informational purposes only. It does not constitute medical advice and should not replace consultation with a licensed healthcare professional. For complete guidance, please review our full disclaimer.













